Peripheral Neuropathy May Indicate Mitochondrial Myopathy
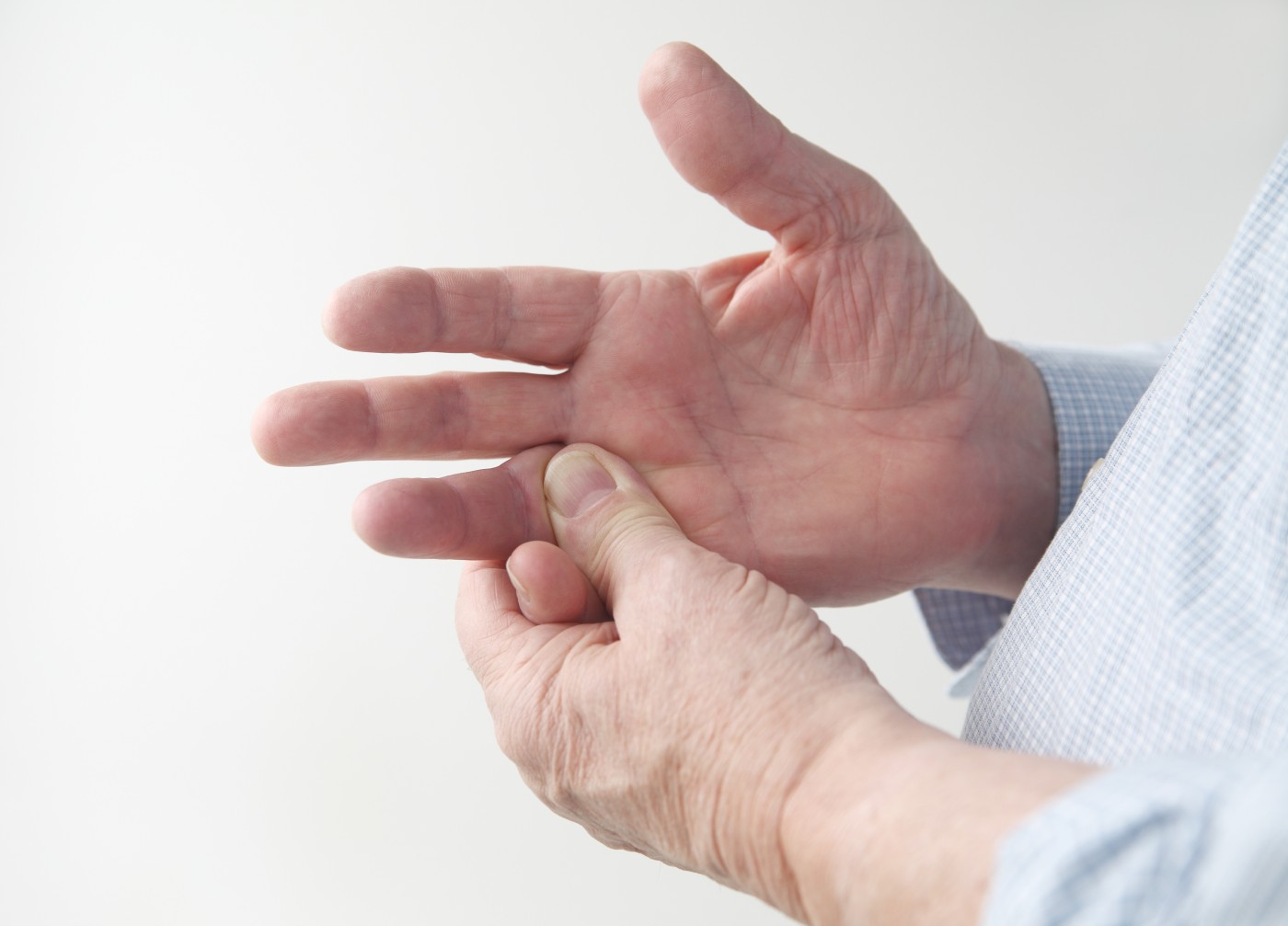
 A simple blood or urine test, rather than an invasive muscle biopsy, may be all that is needed to diagnose mitochondrial disease in patients with peripheral neuropathy (muscle weakness or a pricking sensation in the extremities) and progressive external opthalmoplegia. Researchers from the National Hospital for Neurology and Neurosurgery in London found that the presence of mitochondrial gene mutations was correlated with the presence of peripheral neuropathy and progressive external opthalmoplegia, two clinical manifestations of mitochondrial disease.
A simple blood or urine test, rather than an invasive muscle biopsy, may be all that is needed to diagnose mitochondrial disease in patients with peripheral neuropathy (muscle weakness or a pricking sensation in the extremities) and progressive external opthalmoplegia. Researchers from the National Hospital for Neurology and Neurosurgery in London found that the presence of mitochondrial gene mutations was correlated with the presence of peripheral neuropathy and progressive external opthalmoplegia, two clinical manifestations of mitochondrial disease.
“We suggest that nuclear gene testing may enable a more rapid diagnosis and avoid muscle biopsy in patients with progressive external ophthalmoplegia and peripheral neuropathy,” wrote lead author Dr. Alejandro Horga in the article, “Peripheral Neuropathy Predicts Nuclear Gene Defect in Patients with Mitochondrial Opthalmoplegia,” which was published in Brain. “This observation may facilitate the development of diagnostic algorithms.”
The basis of the study was a retrospective analysis of 116 genetically-defined mitochondrial disease patients with progressive external opthalmoplegia. Dr. Horga and his colleagues paid attention to the records of demographics, clinical data, and neurophysicological data from these patients, as well as the type of mutation present.
Three main types of mutations were found: single mitochondrial DNA mutation (67% of patients), point mutation in mitochondrial DNA (10% of patients), or multiple mitochondrial DNA mutations in muscle without an accompanying nuclear gene defect (22% of patients). Other common mutations were found in the genes POLG, C10orf2, and RRM2B.
Over half of these patients presented with peripheral neuropathy, with the most prevalent occurrence in patients being a point mutation in mitochondrial DNA (44% of patients) or nuclear DNA defects (52% of patients). Significantly fewer (2%) patients with a single mitochondrial deletion had peripheral neuropathy.
Mathematical models and analyses showed that only peripheral neuropathy could independently predict nuclear defects: age at disease onset, gender, family history, progressive external opthalmoplegia at clinical presentation, hearing loss, pigmentary retinopathy, and extrapyramidal features could not predict the mutations. Peripheral neuropathy was highly specific for diagnosing nuclear DNA defects.
Although mitochondrial respiratory diseases are very diverse in their clinical manifestations, it appears as though peripheral neuropathy predicts nuclear DNA defects in patients with progressive external opthalmoplegia. These findings may be used clinically to help diagnose mitochondrial myopathy, where a patient with peripheral neuropathy may be advised to be tested for genetic defects.






